Lipedema, Inflammation and Keto Way of Eating
In this article we are going to explore the relationship between Lipedema, Inflammation and Keto Way of Eating. Despite our years of countless efforts battling the dieting and exercise paradigms, there may just be a means of finally achieving relief for those who suffer from Lipedema and its co-occurring conditions. Read on to see if this may be a solution for you too!
Have your heard or thought the following:
- How did you get so fat?
- Haven’t you tried to diet or exercise to get the weight off?
- You are clearly cheating on your diet?
- You aren’t exercising enough?
- Have you considered bariatric bypass surgery?
- Don’t you have any pride in the way you look?
These are all truly hurtful things to say to anybody and fat shaming should never be tolerated, even by someone in the medical profession! There are many reasons someone may be overweight that do not necessarily involve obesity. A good example is someone suffering from a medical condition like Lipedema! Until you knew you had this adipose fat tissue disease you probably felt pain, shame and hated your body for not being the shape you tried so desperately to achieve. You may have even turned to extreme and unhealthy disordered eating behaviors, such as bulimia, fad diets, diet pills or engaged in dangerous caloric restrictive eating, in an effort to try and lose the excess weight. What you found is none of the aforementioned methods worked on these areas of fat.
Peer pressure and social norms are powerful drains for an already emotionally charged Lipedema woman. Don’t you think I want to look and feel “normal” like everyone else? I want to wear nice clothes, feel sexy, be loved by a partner, go out and be social, have children, and not have to feel the physical and emotional pain of being fat that severely limits what I can do and how I see myself. I’ve tried everything and am almost ready to give up and accept my fate in life.
What if I said you can help improve your body and mind by making some healthy nutritional changes in your life? This is something I discovered and it has already helped me significantly reduce inflammation and pain as well as shed some excess weight. I was able to dropped over 100 pounds, which I have NEVER been able to do before! I was not starving and several other of my comorbidites are improving too! However, most of my weight came back, not due to failure of keto, but to a hypothyroid and other hormonal situation.
Let’s look at Lipedema, Inflammation and Keto Way of Eating!
Understanding Food and Inflammation

Nutrition and eating lifestyles have always been a problem for those with Lipedema. This is particularly true with the modern day American diet that many of us adopted back in the mid to late twentieth century. We were introduced to a rapidly growing market of processed foods, which caused a high intake of saturated fatty acids and trans fatty acids along with chemical preservative names we can’t even pronounce.
We were misinformed, on several levels, about 1) the quantity and types of foods that are actually beneficial (versus being harmful) to keep our bodies functioning in optimal capacity, 2) the quality of the foods, fresh, frozen or processed, and the chemicals used to reproduce, grow, harvest and preserve those foods, and 3) the impacts of ingesting artificial ingredients, especially in quantity over time, and their effects on overall health.
There was also the boom of the fast food markets that provided little to no nutritional value. All of this was in the name of providing time saving convenience for the working family.
The high intake of unhealthy saturated fatty acids, trans fatty acids, sugars (both natural and artificial) and high-glycemic carbohydrates in processed food all contribute to inflammation. Our bodies need plenty of fat, but only the healthy saturated and unsaturated fats. Contrary to a long held belief “eating fat does NOT make you fat!” In fact, we were strongly advised back in the 1980s to eat only a low-fat diet, which has done more harm to our health than anything else to date. (Ask the record number of people having gallbladder removals!)
All these modern conveniences and changes to good clean eating by experts who know little about body function and nutrition, have come at a high price for those of us who suffer with Lipedema and other chronic illnesses! These negative changes in nutrition patterns have caused a rise in digestive problems, which in turn has helped create high levels of inflammation, which can sometimes become persistent. Inflammation can be a bad thing!
Think of your body like a pot of water on the stove. You have been simmering with constant inflammation on low for a while. Then as you continue to eat the wrong foods you raise your inflammation levels, causing that pot of water to now boil in a constant inflamed state. If left to boil the inflammation causes internal damage and will spur new Lipedema masses, create lymphatic flow problems, cause digestive problems in your gut and intestinal tract and a host of other body issues or comorbid conditions.
So, our primary mission is to: 1) recognize the signs of inflammation, 2) outline what causes inflammation, and 3) learn how to eliminate it (or for some of us significantly reduce it).
Signs of Inflammation
Inflammation is the body’s immune system response to an injury or infection. There are typically five signs of inflammation:
- Redness
- Heat
- Swelling
- Pain
- Loss of function (1)

Note that not all five signs need to be present for the body to respond to inflammation. At times only one may be present. For those with Lipedema pain and swelling are our most common persistent signs of ongoing inflammation.
For me personally, my abdomen will bloat, my face and cheeks turn red, my legs will swell, and pain levels will rise. I will also have joint and muscle pain, parts of my body will get hotter to the touch and I will experience such fatigue that I can barely get out of bed. At times, it feels like my whole system will go into a shut down with pain and swelling from head to toe. These are the obvious signs of severe inflammation in my system.
When your system is inflamed your immune system releases inflammatory mediators, such as tissue hormones and histamine, that open up your blood vessels allowing more blood and defense cells into the affected area(s). These defense cells also carry more fluid into the area causing swelling and irritation of nerves, which send pain signals to your brain.
It should be noted in some cases your mast cells, which are the main regulators of your system and are responsible for releasing histamine and other substances during inflammatory and allergic reactions, may go on a rampage and end up causing more inflammation in your body than it resolves. This condition, known as Mast Cell Activation Disease (MCAD) is an observed comorbidity for those with Lipedema. While this condition can cause mild to severe anaphylaxis. there are diagnostic criteria and treatments available to control MCAD.
What Causes Inflammation
In most people with inflammation the cause is usually from an obvious injury or infection. However, for those of us with Lipedema, it is our current way of eating along with stress, medication, smoking and excess unhealthy fat intake that fuels our inflammation. Did you know about 70% of our immune system is housed in our gut? (2) When we disrupt the fine balance of the gut microbiome, we help create inflammation, which can lead to disease, autoimmune problems and chronic digestive problems. If we don’t change our way of eating and lifestyle choices inflammation levels will rise making our Lipedema and other co-occurring conditions worse and more painful. Inflammation is ultimately what is killing us!
One of our biggest enemies is sugar, particularly the processed kind! Sugar, or glucose, acts much like a narcotic in your system creating a “sugar high” when consumed in any quantity. This simple carbohydrate activates your body’s happiness hormones – serotonin, dopamine, and endorphins – that enhances your happiness, minimizes pain perception and overall makes you feel good.
While these feelings may be desirable, the underlying harm to your body is significant. When your body burns glucose (sugar) as its fuel source the hormones that control appetite satiety are never fired, therefore making you feel continually hungry, leading to overeating and increased caloric intake. It also creates a series of spikes and drops in your blood sugar levels giving you the sense of energy abundance for a short period of time followed by a rapid decrease of energy. It creates a damaging cycle of cravings and imbalance in your system, setting you up for insulin insufficiency or resistance issues, which can lead to a high probability of obesity, Type 2 Diabetes and other harmful conditions.

Your body produces a hormone, called insulin, that is responsible for facilitating the conversion of incoming glucose (sugar) into usable fuel that can feed cells from your bloodstream. Insulin is also responsible for directing the storage of excess glucose as fat in your body until it may be needed in the future.
Insulin helps keeps your blood sugar level from getting too high (hyperglycemia) or too low (hypoglycemia), thereby acting as a blood sugar regulator. If your body cannot produce enough insulin or your cells are resistant to the effects of insulin and cannot effectively handle incoming glucose, you are considered insulin resistant. This condition, if not addressed quickly, can lead to hyperglycemia and Type 2 Diabetes.
Consuming excess sugars, which could be just one can of soda, and refined carbohydrates have been linked with increased inflammation markers. A blood test measuring C-reactive protein (CRP) levels can determine how much and how long your body remains inflamed after ingesting these inflammatory carbohydrates. It should be noted that elevated inflammation markers can also be triggered by additional factors outside the consumption of added sugars and refined carbohydrates include factors like stress, medication, smoking and excess fat intake.
Consuming excess added sugars and refined carbohydrates is also linked to serious health issues beyond chronic body inflammation. These include the following:
- Excess production of AGEs: Advanced glycation end products (AGEs) are harmful compounds that form when protein or fat combine with sugar in the bloodstream. Too many AGEs leads to oxidative stress and inflammation.
- Increased gut permeability: Bacteria, toxins and undigested food particles can more easily move out of the gut and into the bloodstream, potentially leading to inflammation. (Also known as “leaky gut” syndrome.)
- Higher “bad” LDL cholesterol: Excess LDL cholesterol has been associated with higher levels of C-reactive protein (CRP), a marker of inflammation.
- Weight gain: A diet rich in added sugar and refined carbohydrates can lead to weight gain. Excess body fat has been linked to inflammation, partly due to insulin resistance. (3)
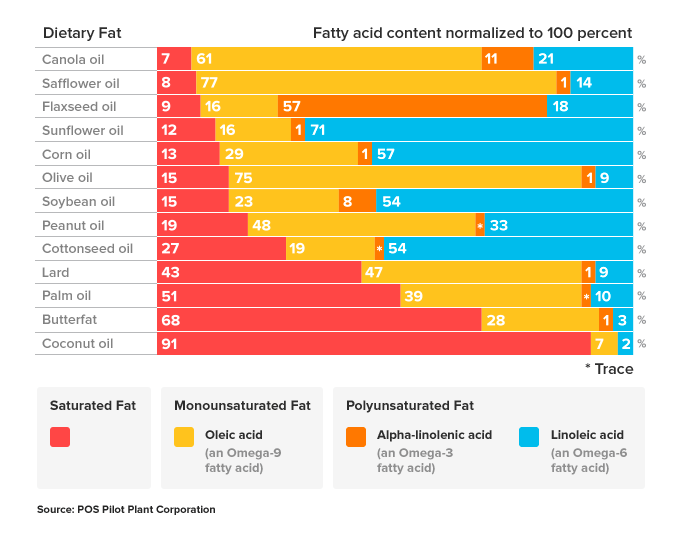
In addition to excess added sugars and refined carbohydrates we also need to be aware our consumption of omega-6 and omega-3 polyunsaturated fats. These fats are essential to our body function and not something our body can produce on its own, so we need to get these nutrients from our diet. It is believed that omega-6s are pro-inflammatory, while omega-3s are anti-inflammatory.
According to health experts we need to maintain a ratio between 4:1 and 1:1 of omega-6 to omega-3 fatty acids in order to derive optimal body benefits and reduce chronic inflammation. Unfortunately, our American diet includes a very high omega-6 consumption rate, pushing the ratio to unhealthy levels, up to 16:1! This high consumption of omega-6 fatty acids, responsible for creating chronic inflammation, may be one of the leading drivers of the most serious modern diseases, including heart disease, metabolic syndrome, Type 2 diabetes, arthritis, Alzheimer’s, dementia and many types of cancers. (4)
How to Reduce Inflammation
As outlined in the previous section, we need to address a couple key chronic inflammation indicators. First, we need to eliminate excess processed sugars from our eating plan. This is easier said than done as added sugar is hidden in many of the foods we ingest every day. Sugar also comes in many forms and names, some we do not readily recognize. Here is a list of 56 common names for added sugars.
It should be noted there is a difference between natural and added sugars. Natural sugars are found in fruits, vegetables and dairy products, which are actually beneficial for you as they offer high fiber content we need in our diet. We still need to evaluate and limit which foods we incorporate in our diet that have natural sugars as we need to keep our blood sugar levels balanced.
#2 – Adjust Omega-6 to Omega-3 Ratios
Second, we need to significantly lower our omega-6 to omega-3 ratio so that it is at or below the recommended 4:1 ratio. We can do that by changing out our ingredient and cooking oils from high omega-6 oils such as corn, safflower, soybean, cottonseed and sunflower oils and choosing healthier omega-3 oils such as butter, coconut, olive, palm, avocado and fish oils.
When considering which version of omega-3 oils to purchase, always choose a “virgin” form instead of a processed or refined version. Refined or processed oils break down faster when cooking, especially at higher heat settings, with some creating harmful or toxic chemicals we actually ingest. This is called the oxidation effect. You definitely need to do your research on choosing good quality oils for both ingredient and cooking purposes to avoid chronic inflammation and unhealthy byproducts from settling in your body! Here is a list of cooking oils and how they affect your health.
#3 – Eat Real Whole Foods
Third, we need to eat real whole food that is organic and non-gmo (genetically modified). Avoid prepared and convenience foods that come in boxes and bags, which are loaded with preservatives, hidden sugars and chemicals that are harmful to your body. Choose fresh (or frozen) vegetables, grass-fed meats, nuts and whole dairy products that offer beneficial fiber content. Avoid pro-inflammatory foods such as:
- All prepared fast food
- Soft drinks (sodas including diet sodas, juices, flavored drinks)
- Alcohol
- Baked goods (pastries, pies, cakes, etc.)
- Margarine
- Non-organic GMO meats, vegetables and fruit
- Farm raised fish
- Soft cheeses
- Food that comes from a box
- Candies and chocolate (dark cacao chocolate above 70% in moderation)
#4 – Modify Our Lifestyle
Fourth, we need to modify our lifestyle to help reduce our body inflammation. This includes reducing our stress levels and adding in a favorite relaxation technique, such as meditation, yoga, pilates, and reiki or engaging in our favorite physical exercise program, such as swimming, cycling or walking. If you smoke now would be a good time to try breaking that bad habit.
If you change your lifestyle and start making positive progress towards reducing inflammation, losing weight and feeling more energized, you may want to revisit the need for certain medications. I am not a doctor and would never advise anyone just stop taking medications for any reason. You should be working with your doctor and nutritionist before and during major lifestyle changes so they can monitor your body changes, medication needs and help you avoid anything that might potentially cause you harm.
#5 – Eliminate Trigger and Allergy Items
Fifth, identify and eliminate any “trigger” foods or foods that produce sensitivities or allergic reactions. These foods or food groups tend to irritate your digestive system and produce painful symptoms, such as bloating, excess gas, diarrhea or constipation, cramping and even bleeding. My blood work came back as allergic to gluten and was diagnosed with Celiac Disease. Once I cut out all gluten products, within 10-12 weeks my system started feeling much better and it was easier for me to transition into a Ketogenic way of eating.
Others who have IBS (irritable bowel syndrome), Crohn’s Disease, Ulcerative Colitis or other gut or bowel condition may also need to incorporate a low-FODMAPs (Fermentable Oligosaccharides, Disaccharides, Monosaccharides and Polyols) into their new food plan. Food on the high FODMAPs list are not necessarily bad foods. It just means these foods feed the wrong bacteria in your system thus producing the aforementioned symptoms. You will need to avoid these foods to give your system time to heal the bacteria imbalance in your gut and intestinal tract. You may be able to add some of them back in the future, but for now, if you have digestive issues you need to be on a low-FODMAPs food plan.
New Way of Eating
Now that we have identified sources of inflammation in our system and ways to reduce that inflammation, how do we identify the best way of eating for those of us with Lipedema? That is the $64,000 question. Food plans are as unique as each of us. The plan I follow may not exactly work for you as I have a set of food allergies and sensitivities I need to incorporate into my new food plan. You may not have those same restrictions or may have a different subset of restrictions that you will need to factor into your plan.

The first thing we need to address is changing the fuel source used to energize our body. If you have been battling inflammation, experiencing blood sugar spikes and drops during the day, feel hungry shortly after eating and battle obesity, mood swings, or chronic digestive or auto-immune diseases then you are probably part of the majority of people who derive their body fuel from glucose (or sugar) sources. This is not a stable reliable source of fuel for your cellular needs and as we have seen it is actually harmful to proper body function over time.
We need to look at the consumption of healthy fats and in turn fatty acids as a more stable energy source for our overall body function. For the past four decades we have been told by various organizations that “fats” are bad for us and we should choose food products that are “low-fat” for a healthy diet. This kicked off a flood of low-fat products in the market, which is one of the key turning points for the underpinning of the obesity epidemic. What essentially happened is the good healthy fats were replaced by artificial sweeteners and chemicals that are actually harmful to our bodies.
Your body needs healthy fats to function properly. It also needs an adequate supply of protein and carbohydrates, known as macro-nutrients, to build and maintain a healthy body. All three of these macro-nutrients need to be consumed in the correct percentage to provide optimal body function and avoid negative consequences such as obesity, chronic disease generation, muscle wasting, organ damage and brain dysfunction. The role of macro-nutrients in the body:
- Proteins: required for building and maintaining tissues and muscles; hormone production; enzyme function; support of immune function; limited energy production.
- Carbohydrates: provides immediate fuel for body use; provides stored energy source for when needed; source of fiber; immediate source of fuel for intense workouts
- Fats: primary source of energy; key for vitamin absorption; maintains body insulation and temperature regulation; healthy fats promote good heart and brain function; signals brain fullness satiety to prevent overeating.
For those with Lipedema we have seen conventional dieting and caloric restrictions do not work! We need to change our way of eating to focus on an anti-inflammatory regimen. What we choose to follow, which is a unique decision for each of us as there is no one-size-fits-all solution, must be sustainable. This means we make this change for life not for a limited period of time as the Lipedema fat, inflammation and pain will re-surge with a vengeance once we return to our old ways!
We still need clinical trials to show what kind of eating plan is the most beneficial to those with Lipedema. However, we have a brand new paper written by Leslyn Keith, Siobhan Huggins and Carrie Reedy of Lipedema Simplified this year (2025) showing the positive effects of a low carbohydrate way of eating for those with Lipedema. It is titled “Therapeutic Carbohydrate Reduction for Lipedema: Guidelines for a Patient-Centered, Holistic Approach.”
The rest of the information presented is based on my personal research and my own experience in trying several eating plans in an effort to find positive change for my severe stage Lipo-Lymphedema condition. It is always recommended you do your own research and determine for yourself which eating plan might work best for your situation. Once you have had done your due diligence, it would be advisable to talk with your doctor and nutritionist about any caveats or concerns in proceeding with your chosen plan.
Now given what we know about how the body uses macro-nutrients, the special needs of those suffering with significant inflammation, swelling and pain of Lipedema, those who desire significant weight loss, and those who desire to eat a healthier diet other than the current American diet, let’s explore two ways of eating with documented success – Ketogenic and Mediterranean plans – starting with the Ketogenic way of eating.
Ketogenic Way of Eating
As we identified above, adequate macro-nutrient consumption is required for health body function. This also includes a proper balance of electrolytes too. However, the type and amount of macro-nutrient consumption is key to how well the body responds and its lasting health effects on our system.
Unfortunately, the Standard American Diet (SAD), which has been degrading for decades now, is responsible for many of the current day diseases and obesity epidemic. As you can see below 50% of our macro-nutrients are coming from carbohydrates, which are mostly sugar and processed food based. Changing our macro-nutrient composition and replacing sugar, processed and fast food items with real whole food can make a profound effect on our body function and health, not to mention our waistline!
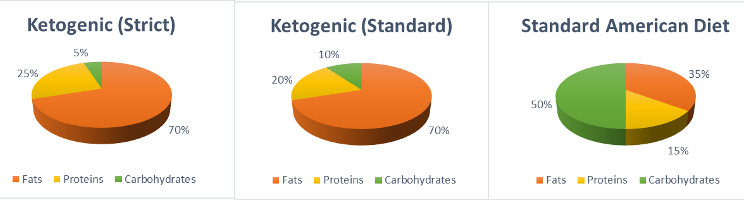
Let’s look how changing our macro-nutrient composition and the quality of our food addresses our overall health. Hopefully you will see we can reclaim an improved quality of health while reversing crippling health conditions and addressing our current obesity epidemic!
The Ketogenic eating plan has the most documented success of any anti-inflammatory plan so far! A Ketogenic plan derives its name from the ketones produced when your body, specifically the liver, converts ingested fats into fuel.
The main highlights of a Ketogenic or Keto eating plan are:
- Low carbohydrate intake
- Moderate protein intake
- High fat intake
- Energy source from fats via ketones rather than carbohydrates
- Sustained energy throughout the day (without spikes and drops in blood sugar)
- Fullness/satiety
- Weight loss even without exercising* (bonus!)
*Note: no one is advocating to stop exercising. You don’t need to be a professional athlete, but at the minimum we need to keep our muscles toned.
Macro-nutrient Makeup
A Keto plan focuses on eating real whole food. Carbohydrates should be no more than 5-10% of your daily intake and ideally between 20 and 50 grams per day. (Here is a great visual to illustrate the difference in food items available on both a 20 gram and 50 gram carbohydrate plan.) Your carbohydrates are mainly consumed through cruciferous vegetables and foods high in fiber content. Avoid carbohydrates that contain starches, all grains, pastas and rices. Most fruits are high in natural sugars and should be avoided. Beneficial fruits include avocados, coconut, berries, lemons, limes, olives and rhubarb.
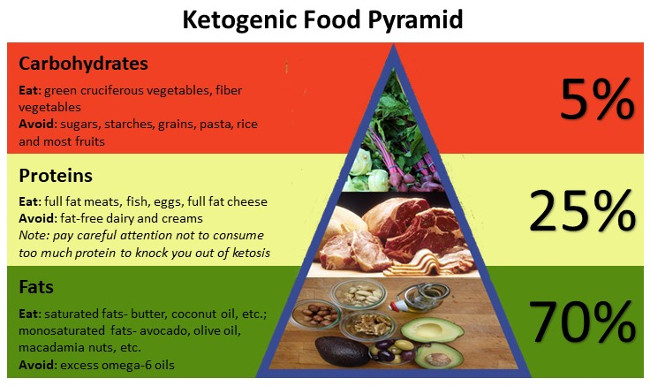
Protein intake should include full whole meats and fish including the fatty portions, organ meats, eggs preferably cage-free, and full fat cheeses like block cheddars and cream cheeses. Fish selections are not only naturally low in carbohydrates but also contain good levels of valuable omega-3 oils. Ideally daily protein intake should be 1.2 to 1.5 grams per your daily body weight measured in kilograms. (For example, an ideal weight of 180 pounds or 81.6 kilograms would consume between 98 and 122 grams daily.)
Including an adequate amount of healthy fats each day is important to achieving and maintaining the state of ketosis, which is the body’s means of converting food into ketones that is used as fuel for sustaining body energy. As we examined above there are good and bad fats. We definitely want to limit our intake to the healthy fats that provide low omega-6 and higher omega-3 levels. Try changing out your cooking and ingredient oils to virgin olive, avocado, peanut. coconut oils and butter or ghee. Also include healthier nuts and seeds like macadamia, pecan, and brazil nuts for snacks and as ingredients.
Items to avoid on a keto plan include alcohols, sugary drinks, foods labelled as “low-carb” or “low-fat” which are actually high in sugars, artificial sweeteners, foods high in starch and fruits high in sugars. The DietDoctor has a good list of which foods to include and exclude when changing over to a keto way of eating.
Nutritional Supplements

When you switch from a glucose to fat burning methodology you need to be aware of changes to your electrolyte levels to ensure your body does not experience a deficiency that could cause adverse effects on body functions. Electrolytes are substances required by the body to carry electrical energy for communication between an affected area and the brain. They commonly include sodium, which is probably the most common deficiency seen, magnesium, potassium, calcium and phosphate.
When modifying your way of eating to a keto plan you need to be sure to include plenty of foods that provide adequate levels of electrolytes and how to remedy them if you have a temporary deficiency. If you suspect any ongoing symptoms of a deficiency please consult your physician or registered nutritionist for possible supplement information.
Sodium
- Recommended – 3 – 7 g of sodium (7 – 17 g of salt, i.e. 1-3 teaspoons)
- Symptoms – includes fatigue, weakness, headaches and trouble concentrating
- Actions – be sure to include salt liberally in your cooking and on your food. You can also eat pickles or olives that are high in salt or drink a cup of bouillon or bone broth daily. In rare cases your doctor may prescribe salt tablets for those with severe sodium deficiency.
Potassium
- Recommended – 3,000–4,700 mg daily
- Symptoms – muscle cramps or twitching, heart palpitations or hearing your heartbeat louder than usual
- Actions – eat more avocados, chards, mushrooms, spinach, brussel sprouts or broccoli. (Check with a doctor if a deficiency is suspected.)
Magnesium
- Recommended – 400 mg magnesium
- Symptoms – muscle twitching or cramping especially at night or after exercising
- Actions – eat hemp seeds, swiss chard, pumpkin seeds, mackerel, chia seeds and dark chocolate. (7)
Taking any over the counter supplements should be discussed with your physician or nutritionist before starting a regimen. You should try to get all your nutritional needs through natural whole foods whenever possible.
In addition to the identified electrolytes, don’t forget to keep up on your water intake too!
The Keto Flu
During the initial couple of weeks of switching to a Keto way of eating your body may experience electrolyte imbalances (headaches, trouble concentrating, mood swings, sugar cravings, muscle cramps, etc.) as described above along with bowel changes. It’s called the “Keto flu.” It is not really a flu, but produces temporary symptoms like a flu. Here is another source of “remedies” that you can use to help mitigate the symptoms of the “Keto flu.”
This is normal for those during the adaptation period and can be mitigated fairly quickly by making sure your electrolyte levels are met each day and sticking to a strict Keto eating plan. During this adaptation period you will likely lose more water and sodium than normal. Symptoms and the length of the “Keto flu” vary from person to person but the symptoms are generally the same.
To help you mitigate the “Keto flu” monitor your sodium and water intake. You may need to increase their intake for the first week or so until the flu phase passes. Try to limit physical activity where electrolytes and water can be lost quickly.
You may also have to ease into the Keto plan by eating 50 grams of carbohydrates for the first week or two until you can work your way down to 20 grams per day. You might hear people refer to this as “dirty”, “sloppy” or “lazy” keto. (I had to do this for a bit to mitigate my symptoms.)
Don’t worry about calories during this period and eat full healthy meals.
Ready for a New Way of Eating?
Changing your way of eating can feel daunting and overwhelming not knowing where to start with creating healthy meals. Fortunately, there are many online resources and books loaded with new and exciting recipes to get your new way of eating off to a good start.
I am personally trying new dishes and learning what works for my family and myself. Once you learn the basics of what type of foods to include, you can make a plethora of dishes that meet your dietary needs all while creating a healthier version of you! And as a great side effect, you will lose weight and boy do I need to lose quite a bit of weight! And let’s now forget this eating plan significantly reduces inflammation and body pain, which can heal quite a few conditions and diseases. I know I already feel so much relief from the constant and severe pain from Lipo-Lymphedema, Celiac Disease, MCAS, leaky gut and osteoarthritis to name a few!
I will also note once you are adapted to the Keto way of eating you will notice how different real food tastes and how bad sugar and sweets now taste! It’s amazing how wired your brain and taste buds become when you ingest high levels of sugars and carbohydrates. The cravings can be intense. It’s almost akin to going through a drug withdrawal and it changes your outlook on food once you are fully adapted to a Keto way of eating!
Keto Stall or Plateau?
If you feel your weight loss has stopped despite continuing to eat a keto plan, check out 13 Reasons Keto May Not Be Working for You for tips on how to jumpstart your weight loss and achieve your health goals.
Keto Resources
Videos on Keto Way of Eating for those with Lipedema:
- Lipedema & Keto | Leslyn Keith, OTD & Catherine Seo, PhD
- Diet Doctor – A keto diet for beginners
- Fat Disorders Resource Society – Comparing Nutrition Plans for the Lipedema
- Keto Diet + Carb Cycling w/ David Jockers, DC
- Ketogenic Way of Eating for Lymphatic Disorders – Dr. Eric Westman – LE&RN
Websites:
- DietDoctor.com (comprehensive site for information, recipes, meal plans, etc.)
- Healthline – 16 Foods to Eat on a Ketogenic Diet
- DrBerg.com – Keto Diet Plan
- Lipedema Simplified – A Keto Way of Eating for Lipedema
- Facebook: Keto & Low Carb Recipes for Beginners
- Facebook: Lipedema & KETO Way of Eating
- Facebook: Keto Recipes for Beginners
Understanding the differences in eating plans, the commitment involved in sticking with the plan and determining your specific health and nutrition goals are the first steps in deciding which plan works best for your individual needs. Everyone is different and there is no one-size-fits-all solution. Follow the rules of the plan and listen to your body. Only you can determine what is successful for your body and help create a healthier version of you!
I hope you were able to learn more about Lipedema, Inflammation and Keto Way of Eating to see if it is a fit for your health goals!
Coming up next… the Carnivore, Ketovore and Mediterranean way of eating plans, See my information on Intermittent Fasting too.
To Your Improved Health!
References:
- (1) U.S. National Library of Medicine: PubMed Health – What is Inflammation?
- (2) US National Library of Medicine National Institutes of Health – Allergy and the Gastrointestinal System
- (3) Healthline – Does Sugar Cause Inflammation in the Body?
- (4) Healthline – How to Optimize Your Omega-6 to Omega-3 Ratio
- (5) Dr J. – The Good, The Bad, and the Ugly Fats
- (6) US National Library of Medicine National Institutes of Health – Ketogenic diets as an adjuvant cancer therapy: History and potential mechanism
- (7) DietDoctor.com – Do you need electrolyte supplementation on a keto diet?
Resources:
- Lidsen Publishers – Therapeutic Carbohydrate Reduction for Lipedema: Guidelines for a Patient-Centered, Holistic Approach
- US National Library of Medicine National Institutes of Health (PubMed) – The importance of the ratio of omega-6/omega-3 essential fatty acids
- The Real Skinny on Fat (multi-part video series)
- Greatist – The 100-Percent Rule: The Simple Advice That Changed My Life
- Facebook – Lipedema and Keto Way of Eating (closed group)
- Facebook – Fat Disorders Resource Society
- Lipedema Project – Keto Way of Eating and Lipedema
- Medium – Salt Scam
- Evolving Wellness – How to Choose A Coconut Oil: Comparing Best and Worst Brands

Learn a lot of stuff today about lipedema inflammation and how to do the keto way of eating.Nice content, good read and informative.
I am so glad you found the information helpful! Eating a low carbohydrate diet has proven effects of reducing the pain, inflammation and size of lipedema in the body. I have personally experienced the positive effects of eating low carbohydrate or keto with significantly reduced pain, reduced swelling and weight loss. What we eat certainly has a huge impact on our overall physical and mental health, never mind the positive things it can do for those who suffer with lipedema or lipo-lymphedema!
Esther